Introduction
Blood products are lifesaving therapeutic tools used in modern medicine to manage bleeding, anemia, clotting disorders, trauma, surgeries, and critical illnesses. Rather than transfusing whole blood in most situations, current medical practice relies on specific blood components tailored to the patient’s needs. This targeted approach improves safety, effectiveness, and resource utilization.
Understanding blood products is essential for anyone involved in patient care. Knowing what each product contains, when to use it, and what complications to watch for can significantly improve patient outcomes. In this article, we will explore the major blood products, their composition, indications, practical decision-making algorithms, and potential complications.
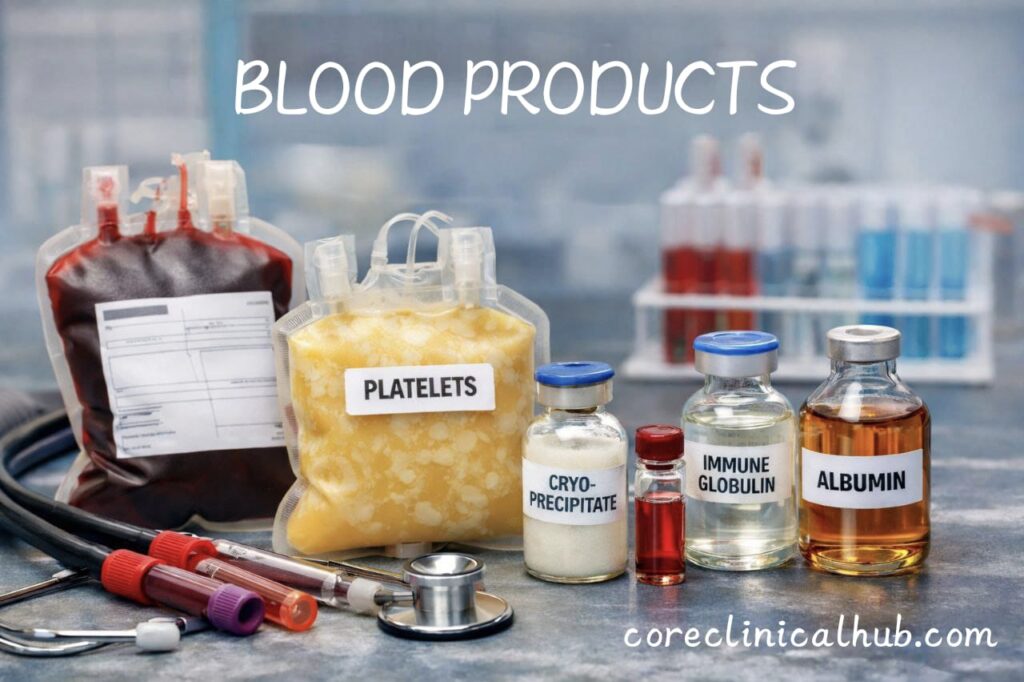
What Are Blood Products?
Blood products are components separated from donated whole blood or manufactured from plasma derivatives. After collection, blood is processed into different components such as red cells, platelets, plasma, and cryoprecipitate. Each component has specific indications based on the patient’s clinical condition.
Blood transfusion therapy today is component-based rather than whole-blood-based because:
- It reduces unnecessary exposure to unwanted components
- It minimizes complications
- It allows efficient use of donated blood
- It enables treatment of specific deficiencies
Types of Blood Products
The six essential blood products you must know include:
- Packed Red Blood Cells (PRBCs)
- Platelet Concentrate
- Fresh Frozen Plasma (FFP)
- Cryoprecipitate
- Whole Blood
- Plasma Derivatives (e.g., Albumin, Immunoglobulins, Clotting Factors)
Let us understand each in detail.
1. Packed Red Blood Cells (PRBCs)
Description
Packed red blood cells are concentrated red cells obtained after removing most of the plasma from whole blood. They primarily contain hemoglobin-rich red cells responsible for oxygen transport.
One unit typically raises hemoglobin by approximately 1 g/dL in an average adult.
When to Use PRBCs
PRBCs are used to improve oxygen-carrying capacity in:
- Symptomatic anemia
- Acute blood loss
- Major trauma
- Post-surgical blood loss
- Chronic anemia with symptoms like fatigue, dyspnea, or chest pain
- Hemoglobin below transfusion thresholds (usually <7 g/dL in stable patients, <8 g/dL in cardiac patients)
Important Note
PRBCs are not used for volume expansion alone. If the patient only needs fluids, crystalloids or colloids are preferred.
2. Platelet Concentrate
Description
Platelets are small cell fragments that play a vital role in blood clotting. Platelet concentrates are prepared either from pooled donor platelets or via apheresis.
One unit of platelet concentrate typically increases platelet count by about 30,000–50,000/µL in adults.
When to Use Platelets
- Platelet count <10,000/µL (even without bleeding)
- Platelet count <20,000/µL with risk factors (fever, infection)
- Active bleeding with platelet count <50,000/µL
- Before invasive procedures if platelet count <50,000/µL
- Major surgery or trauma
- Massive transfusion protocols
When NOT to Use
Platelets are generally not useful in conditions like immune thrombocytopenia unless life-threatening bleeding is present.
3. Fresh Frozen Plasma (FFP)
Description
Fresh frozen plasma contains all clotting factors, albumin, and plasma proteins. It is separated and frozen shortly after donation to preserve coagulation factors.
When to Use FFP
- Active bleeding with prolonged PT/INR or aPTT
- Liver disease with coagulopathy
- Disseminated intravascular coagulation (DIC)
- Massive transfusion
- Urgent reversal of warfarin (if specific reversal agents are unavailable)
- Plasma exchange in certain conditions
When NOT to Use
FFP is not indicated for simple volume replacement or mild INR prolongation without bleeding.
4. Cryoprecipitate
Description
Cryoprecipitate is derived from plasma and is rich in:
- Fibrinogen
- Factor VIII
- von Willebrand factor
- Factor XIII
It is mainly used to correct fibrinogen deficiency.
When to Use Cryoprecipitate
- Fibrinogen level <100–150 mg/dL with bleeding
- DIC with low fibrinogen
- Massive hemorrhage
- Certain inherited clotting disorders (if specific concentrates unavailable)
5. Whole Blood
Description
Whole blood contains red cells, plasma, platelets, and clotting factors. It is less commonly used today but may be preferred in certain emergency or trauma settings.
When to Use Whole Blood
- Massive hemorrhage
- Trauma resuscitation
- Situations where component therapy is not readily available
Whole blood provides balanced resuscitation but requires careful matching.
6. Plasma Derivatives
These are purified products derived from plasma.
a) Albumin
Used for:
- Severe hypoalbuminemia
- Large-volume paracentesis
- Burns
- Certain shock states
b) Immunoglobulins
Used in:
- Immune deficiencies
- Autoimmune disorders
- Certain infections
c) Specific Clotting Factor Concentrates
Used in:
- Hemophilia
- Factor deficiencies
- Warfarin reversal (Prothrombin Complex Concentrate)
Which Blood Product to Use? A Practical Approach
Selecting the correct blood product depends on identifying the underlying problem.
| Clinical Problem | Product to Use |
| Low hemoglobin with symptoms | PRBC |
| Low platelets with bleeding | Platelets |
| Prolonged INR with bleeding | FFP |
| Low fibrinogen | Cryoprecipitate |
| Massive trauma | Whole blood or balanced components |
| Specific factor deficiency | Factor concentrate |
Clear Algorithm for Blood Product Selection
Step 1: Assess Clinical Status
- Is the patient bleeding?
- Is there hemodynamic instability?
- What are the laboratory findings?
Step 2: Check Key Lab Values
- Hemoglobin
- Platelet count
- PT/INR
- aPTT
- Fibrinogen
Step 3: Match the Defect
- Low Hb → PRBC
- Low Platelets → Platelet transfusion
- High INR with bleeding → FFP
- Low fibrinogen → Cryoprecipitate
- Massive bleeding → Activate massive transfusion protocol
Step 4: Reassess
Repeat labs after transfusion to evaluate response.
Conditions Requiring Blood Products
1. Trauma
Massive blood loss may require PRBCs, plasma, and platelets in balanced ratios.
2. Surgical Bleeding
Component therapy based on lab parameters.
3. Obstetric Hemorrhage
Rapid transfusion protocols with attention to fibrinogen levels.
4. Liver Disease
FFP and cryoprecipitate may be needed.
5. Bone Marrow Disorders
Platelet and red cell transfusions.
6. Cancer Therapy
Chemotherapy-induced cytopenias.
Complications of Overuse or Mismatched Use
While blood products save lives, inappropriate use can cause serious harm.
1. Acute Hemolytic Transfusion Reaction
Occurs due to ABO incompatibility. It can cause shock, kidney failure, and death.
2. Febrile Non-Hemolytic Reaction
Common and usually mild.
3. Allergic Reactions
Ranging from mild rash to severe anaphylaxis.
4. Transfusion-Related Acute Lung Injury (TRALI)
Severe lung injury within 6 hours of transfusion.
5. Transfusion-Associated Circulatory Overload (TACO)
Fluid overload causing respiratory distress.
6. Infections
Rare but possible transmission of viral or bacterial infections.
7. Iron Overload
Seen in repeated PRBC transfusions.
8. Electrolyte Imbalance
Hyperkalemia or hypocalcemia during massive transfusion.
Preventing Complications
- Strict blood group matching
- Crossmatching before transfusion
- Careful patient identification
- Monitoring during transfusion
- Using transfusion only when clearly indicated
- Following institutional transfusion protocols
Massive Transfusion Protocol (Brief Overview)
In cases like major trauma:
- Rapid assessment
- Balanced transfusion (e.g., 1:1:1 ratio of PRBC:Plasma:Platelets)
- Monitor calcium levels
- Monitor coagulation profile
- Avoid hypothermia
- Frequent reassessment
Special Considerations
Pediatric Patients
Lower volume thresholds and weight-based dosing.
Elderly Patients
Higher risk of circulatory overload.
Cardiac Patients
Higher hemoglobin threshold for transfusion.
Conclusion
Blood products are indispensable in modern healthcare. Each component has a specific role and must be used judiciously. The key to safe transfusion practice lies in understanding the underlying deficiency, choosing the appropriate product, and monitoring carefully for complications.
Rational and evidence-based use of blood products not only improves patient outcomes but also preserves precious donated resources. Mastery of blood component therapy ensures that lifesaving interventions are delivered safely and effectively.
Frequently Asked Questions (FAQs)
What is the difference between whole blood and PRBC?
Whole blood contains all components, while PRBC contains mostly red cells with minimal plasma.
When should hemoglobin trigger transfusion?
Typically below 7 g/dL in stable patients, or below 8 g/dL in cardiac patients.
Can FFP correct anemia?
No. FFP contains clotting factors, not sufficient red cells to correct anemia.
What is the minimum platelet count required before surgery?
Usually 50,000/µL for most surgeries.
Why is cryoprecipitate given in DIC?
Because fibrinogen levels drop significantly in DIC.
What is the most dangerous transfusion reaction?
Acute hemolytic transfusion reaction due to ABO mismatch.
Can blood transfusion cause infection?
Yes, but screening has made it very rare.
What is TRALI?
A serious lung injury occurring within hours after transfusion.
How is massive transfusion defined?
Replacement of a patient’s entire blood volume within 24 hours or large-volume transfusion in a short period.
Is blood transfusion always necessary for anemia?
No. Mild anemia can often be treated with iron or other medical therapy without transfusion.
