Introduction
Chronic Kidney Disease (CKD) is a long-term condition in which the kidneys gradually lose their ability to function properly. The kidneys are vital organs responsible for filtering waste products, balancing fluids and electrolytes, regulating blood pressure, activating vitamin D, and producing hormones that help make red blood cells. When kidney function declines slowly over months or years, harmful substances accumulate in the body, leading to serious health complications.
CKD is often called a “silent disease” because early stages usually produce no obvious symptoms. Many people remain unaware of kidney damage until it becomes advanced. Early detection and proper management can significantly slow progression and reduce complications.
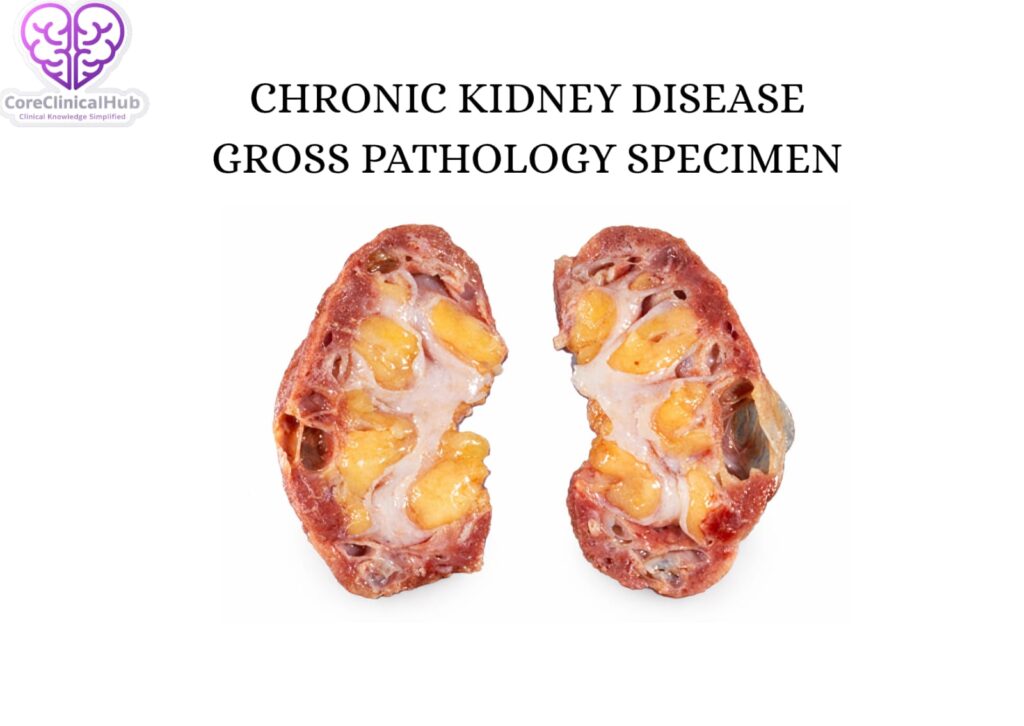
About Chronic Kidney Disease (CKD)
Chronic Kidney Disease refers to structural or functional abnormalities of the kidneys that persist for more than three months. It is characterized by either:
- Reduced glomerular filtration rate (GFR), or
- Evidence of kidney damage such as protein in the urine
CKD progresses gradually and is categorized into stages based on the estimated glomerular filtration rate (eGFR). As kidney function declines, the body struggles to maintain internal balance, affecting multiple organ systems including the heart, bones, and blood.
The disease can affect individuals of all ages, but it is more common in older adults and those with chronic medical conditions.
Risk Factors
Several factors increase the likelihood of developing CKD:
1. Diabetes Mellitus
Persistently high blood sugar damages the tiny blood vessels in the kidneys.
2. Hypertension
Uncontrolled high blood pressure causes strain and scarring in kidney tissues.
3. Family History
Genetic predisposition increases susceptibility.
4. Cardiovascular Disease
Heart and blood vessel disorders are closely linked with kidney health.
5. Obesity
Excess body weight increases kidney workload.
6. Smoking
Reduces blood flow and worsens kidney damage.
7. Long-term Use of Certain Medications
Frequent use of painkillers (NSAIDs) and some antibiotics may contribute to kidney injury.
8. Autoimmune Disorders
Conditions like lupus may attack kidney tissues.
Early identification of these risk factors helps in prevention and timely monitoring.
Signs and Symptoms
CKD symptoms vary depending on the stage. Early stages may show no noticeable changes.
Early Stage Symptoms
- Mild fatigue
- Slight swelling in feet
- Increased urination at night
Moderate Stage Symptoms
- Persistent tiredness
- Loss of appetite
- Nausea
- Muscle cramps
- Puffiness around eyes
Advanced Stage Symptoms
- Severe swelling (edema)
- Shortness of breath
- Confusion
- Persistent vomiting
- Chest pain (due to fluid accumulation)
- Decreased urine output
Because symptoms appear late, routine screening is important for high-risk individuals.
Causes
CKD develops when kidney tissues are damaged over time. Major causes include:
1. Diabetic Kidney Disease
High glucose damages filtering units (glomeruli).
2. Hypertensive Nephrosclerosis
Chronic high blood pressure causes scarring.
3. Glomerulonephritis
Inflammation of kidney filtering structures.
4. Polycystic Kidney Disease
Inherited disorder causing cyst formation.
5. Chronic Obstruction
Long-standing blockage from kidney stones or enlarged prostate.
6. Recurrent Kidney Infections
Repeated infections can lead to scarring.
7. Autoimmune Disorders
Immune-mediated damage to kidney tissue.
Diagnostic Criteria
CKD is diagnosed when abnormalities persist for more than three months. The key criteria include:
- eGFR less than 60 mL/min/1.73 m², OR
- Evidence of kidney damage such as:
- Proteinuria (albumin in urine)
- Abnormal imaging
- Structural abnormalities
- Kidney biopsy findings
Persistent findings over time confirm chronic disease rather than temporary kidney injury.
Diagnosis
Evaluation of CKD involves several investigations:
1. Blood Tests
- Serum creatinine
- Estimated GFR
- Electrolyte levels
- Hemoglobin
2. Urine Tests
- Urine albumin-to-creatinine ratio (ACR)
- Routine urine analysis
3. Imaging Studies
- Ultrasound to assess kidney size and structure
4. Kidney Biopsy
Performed in selected cases to determine the exact cause.
Regular monitoring helps assess progression and treatment response.
Stages of CKD
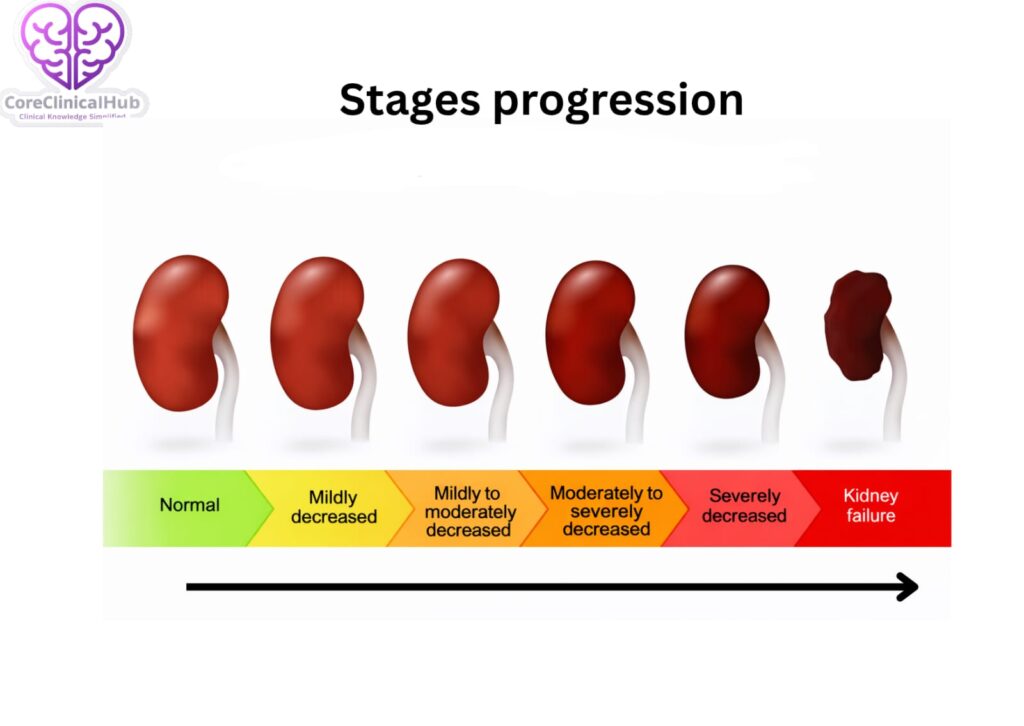
CKD is classified into five stages:
| Stage | eGFR(mL/min/1.73 m²) | Descriptor |
| Stage 1 | ≥90 | Kidney damage with normal function |
| Stage 2 | 60 – 89 | Mild decrease |
| Stage 3a | 45 – 59 | Mild to moderate decrease |
| Stage 3b | 30 – 44 | Moderate to severe decrease |
| Stage 4 | 15 – 29 | Severe decrease |
| Stage 5 | <15 | Kidney failure |
Progression is not inevitable. Many patients remain stable for years with proper care.
Complications
CKD affects multiple body systems. Common complications include:
1. Anemia
Reduced erythropoietin production decreases red blood cells.
2. Bone Disease
Imbalance in calcium and phosphorus weakens bones.
3. Cardiovascular Disease
Heart attack and stroke risk increases significantly.
4. Fluid Overload
Leads to swelling and breathlessness.
5. Electrolyte Imbalance
High potassium can cause dangerous heart rhythm problems.
6. Metabolic Acidosis
Excess acid buildup in blood.
7. Malnutrition
Loss of appetite and protein imbalance.
Early management reduces these risks.
Treatment
CKD management focuses on slowing progression and treating complications.
1. Control of Underlying Causes
- Strict blood sugar control in diabetes
- Blood pressure control (target usually <130/80 mmHg)
2. Medications
- ACE inhibitors or ARBs for kidney protection
- Diuretics for swelling
- Phosphate binders
- Erythropoiesis-stimulating agents for anemia
3. Lifestyle Modifications
- Smoking cessation
- Regular physical activity
- Weight management
4. Management of Electrolytes
Monitoring potassium, sodium, and phosphorus levels.
5. Advanced Therapy
In stage 5 CKD:
- Hemodialysis
- Peritoneal dialysis
- Kidney transplantation
Early planning improves outcomes.
Diet in CKD
Nutrition plays a critical role in slowing progression and managing symptoms.
1. Protein Intake
Moderate restriction may reduce kidney workload.
2. Sodium Restriction
Limit salt to control blood pressure and swelling.
3. Potassium Control
Avoid high-potassium foods in advanced stages.
4. Phosphorus Restriction
Limit dairy and processed foods if levels are high.
5. Fluid Management
Fluid intake may need adjustment in later stages.
Example:
A patient with stage 3 CKD and hypertension may be advised:
- Low-sodium diet
- Moderate protein intake
- Regular monitoring of potassium
A renal dietitian can individualize meal plans.
Preparing for Your Appointment
Patients can optimize medical visits by:
- Bringing previous lab reports
- Listing current medications
- Tracking blood pressure readings
- Noting symptoms and duration
- Asking about stage, progression, and diet
Being informed empowers better decision-making.
Prevention
Although not all cases are preventable, risk can be reduced by:
- Maintaining healthy blood sugar levels
- Controlling blood pressure
- Avoiding unnecessary painkiller use
- Staying hydrated
- Regular screening if high risk
- Maintaining healthy weight
Early detection significantly slows progression.
Prognosis
CKD progression varies widely. Some individuals remain stable for years, while others may progress faster. Factors influencing prognosis include:
- Level of blood pressure control
- Blood sugar control
- Degree of proteinuria
- Lifestyle habits
- Adherence to treatment
With modern management, many patients live long and productive lives.
Reference
This article is based on standard nephrology principles, international kidney disease classification guidelines, and current clinical management practices widely accepted in medical literature.
Frequently Asked Questions (FAQs)
What is the earliest sign of CKD?
Often there are no symptoms. Protein in urine is usually the first detectable sign.
Can CKD be reversed?
Chronic damage cannot usually be reversed, but progression can often be slowed significantly.
Is CKD the same as kidney failure?
No. Kidney failure is the final stage (Stage 5) of CKD.
How often should high-risk individuals get screened?
At least once a year, or more frequently if advised by a healthcare provider.
Does drinking more water cure CKD?
No. Proper hydration helps overall health but does not cure chronic kidney damage.
Can CKD cause heart problems?
Yes. Cardiovascular disease is a major complication of CKD.
Is dialysis permanent?
It may be long-term unless a kidney transplant is performed.
What foods should be avoided in CKD?
High-sodium, high-potassium, and high-phosphorus foods may need restriction depending on stage.
Can young people develop CKD?
Yes, especially if they have diabetes, genetic disorders, or autoimmune diseases.
How is CKD different from acute kidney injury?
Acute kidney injury occurs suddenly and may be reversible, while CKD develops slowly and persists longer than three months.
